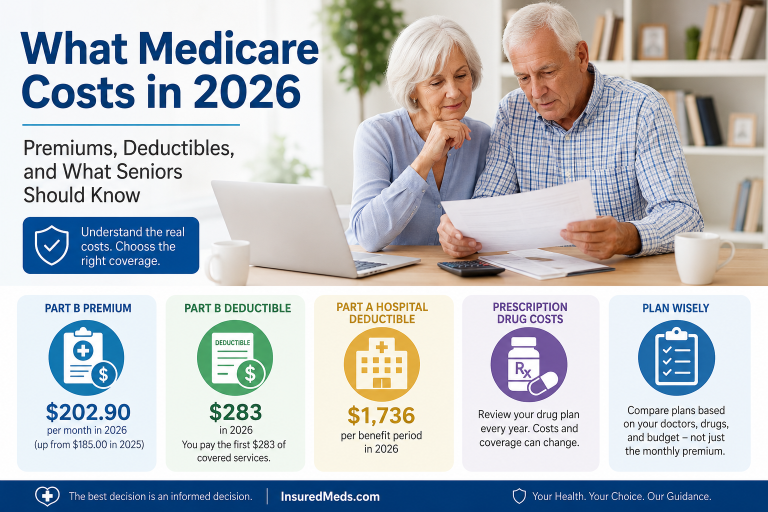
What Medicare Costs in 2026: Premiums, Deductibles, and What Seniors Should Know
Medicare is not free. That surprises a lot of people when they first turn 65. After paying into the system for decades, many seniors assume Medicare will simply take over and cover everything. Unfortunately, that is not how it works. Medicare helps tremendously, but there are still premiums, deductibles, copays, coinsurance, drug costs, and possible…